The Longest Shortest Time
EPISODE #110: Risky Birth-ness
When you give birth by cesarean, doctors are required by law to inform you about the risks—just like they do with any surgery. But when it comes to the risks of vaginal birth, what you’ll hear from your doctor is really up in the air. Some doctors tell patients nothing at all. And many doctors are not even trained to learn about pelvic floor disorders.
 All of this is stunning, because birth injuries, from minor to severe, occur in more than half of vaginal births.
All of this is stunning, because birth injuries, from minor to severe, occur in more than half of vaginal births.
Today, we’re dedicating our entire episode to an interview with Kiera Butler (left), senior editor of Mother Jones, who wrote an article for the magazine about how birth injuries impact women’s lives in profound ways, why we’re seeing an uptick in traumatic births, and most importantly, what you can do to get help if you’ve suffered an injury.
This topic hits particularly close to home because my own birth injury is what led me to start this podcast in the first place. Hear the episode where I process what happened to me—and how that led me to confront Ina May Gaskin, figurehead of the natural birth movement. (Btw, Ina May is in the process of revising her book Ina May’s Guide to Childbirth thanks to the hundreds of comments you left on that post!)
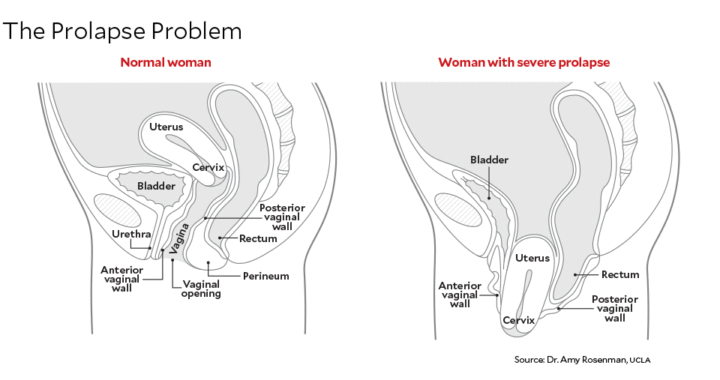
Prolapse is one example of a severe birth injury, in which the uterus or bladder sags
First steps for treating birth injuries
After researching this article and speaking with dozens of doctors, Kiera recommends two first steps in getting treated for pelvic floor injuries:
If you’re in severe pain or discomfort, see a urogynecologist. The American Urogynecologic Society is a great resource to learn more about pelvic floor disorders and to find providers.
Often your issue can be resolved without surgery. So be sure you also consult a pelvic floor physical therapist. Find one through The American Physical Therapy Association.
Pelvic floor PT is a cornerstone of French postpartum care (which sometimes includes dildo video games!).
We also have an episode all about pelvic floor PT here.
Resources for specific postpartum issues
The Association for Pelvic Organ Prolapse Support is a good place to start if you are suffering from prolapse.
The National Association for Continence has some good info on incontinence.
If you’re looking for mental health resources, PATTch is a collective of birth and mental health experts dedicated to the prevention and treatment of traumatic childbirth.
Resources for delivery by cesarean
C-sections save the lives of mothers and babies every day. But just like vaginal births, they carry risks.
The American College of Obstetricians and Gynecologists and the Society for Maternal-Fetal medicine published these guidelines for safe c-sections.
The International Cesarean Awareness Network (ICAN) is a nonprofit organization whose mission is to improve maternal-child health by preventing unnecessary cesareans through education, providing support for cesarean recovery, and promoting Vaginal Birth After Cesarean (VBAC).
This is all meant to inform, not frighten!
Information is power. We can’t predict what will happen when we go into labor, but we can make educated decisions about our bodies and our babies. We hope that the above information is stuff you can keep in your back pocket in the event that you need to use it.
For more real-talk about pregnancy and childbirth, we recommend Childbirth Connection.
What do you wish YOU had known before giving birth?
How could your health care providers inform you better? What’s helped? More resources welcome!
Kiera headshot: Tristan Spinski
Our sponsors for this episode are Squarespace (LONGSHORT), Thirdlove, Yogi Teas, 1-800 Flowers (click Radio Icon enter code LONGSHORT) and Tweed Wolf. Use the promo codes at checkout for a special discount.
The Longest Shortest Time may earn a small commission from products linked on this site. Using our affiliate links helps support our work.